Eczema and psoriasis are two common skin conditions that affect millions of people worldwide. Both have similar symptoms and can often be mistaken for each other, however they differ in terms of their causes and treatments. Knowing the differences between eczema and psoriasis is important so that you can seek out the best possible treatment to manage your symptoms. In this article we will discuss the main differences between eczema and psoriasis, including their causes, signs and symptoms, diagnosis, treatments, prevention strategies and prognosis.
So what is the difference between eczema and psoriasis
1. What are the common symptoms of eczema?
Eczema is a skin condition that can cause various symptoms depending on the individual. The most common symptom is itchy, dry, red patches of skin which may be scaly and inflamed. In more severe cases blisters may form which will be filled with fluid and may ooze or crust over. Eczema can also cause thickened and darkened areas of skin, particularly in creases such as elbows and knees. In some cases people experience an intense burning sensation along with extreme itchiness. Other signs to look out for include swelling around affected areas, discolouration around the eyes, and a rash appearing anywhere on the body.
2. What are the common symptoms of psoriasis?
Psoriasis is a chronic skin condition that causes red, scaly patches of raised skin to form. Common symptoms of psoriasis include dry and cracked skin, itching and burning sensations, thickened or ridged nails, small scaling spots on the face, scalp or trunk of the body. These patches may also be covered with silvery scales which can flake off easily. Additionally, those affected by psoriasis may experience joint pain due to inflammation caused by the condition. Psoriatic arthritis is a type of joint pain that often affects people with psoriasis as well.
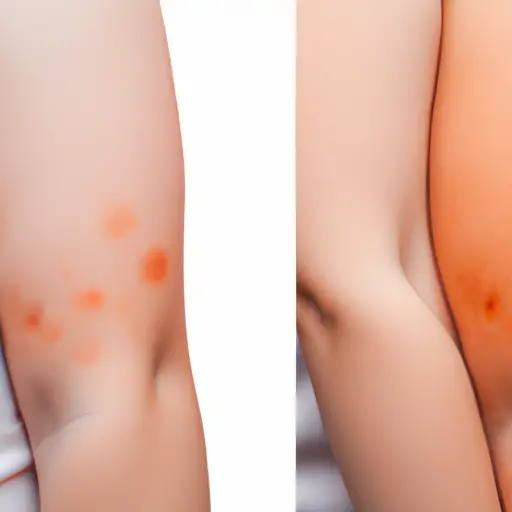
3. How do the two diseases present differently on skin?
Atopic dermatitis and psoriasis are both skin disorders, but they present differently. Atopic dermatitis is a chronic condition that causes dry, itchy skin. It often appears as patches on the face and body, often around the eyes and can worsen with contact to allergens or irritants. Psoriasis is an autoimmune disorder that manifests itself in red patches of thickened skin covered in silvery scales. These lesions typically appear on joints like elbows and knees but can be found anywhere else on the body. The scales may flake off due to itching or scratching, which can cause bleeding and discomfort.
4. Are there any treatments for eczema that don’t work for psoriasis and vice versa?
Yes, there are treatments that work for one but not the other. For example, eczema is often managed with topical ointments and creams containing corticosteroids or calcineurin inhibitors which are not effective for psoriasis. Conversely, light therapy has typically been found to be more successful than creams when it comes to treating psoriasis while having little effect on eczema. Additionally, many natural remedies may provide relief from eczema symptoms but do nothing to mitigate the effects of psoriasis. As such, it is important to receive a proper diagnosis as well as personalized treatment plan that takes into account each individual’s unique medical history and lifestyle factors in order to achieve optimal results.
5. How does a doctor diagnose eczema or psoriasis?
A doctor can diagnose eczema or psoriasis by performing a physical examination and asking questions about the patient’s medical history. The doctor may look for certain signs, such as redness and scaling of the skin, to confirm the diagnosis. If necessary, they may also take a small sample of skin (known as a biopsy) to check whether there are any underlying conditions that could be causing the symptoms. Blood tests may be taken to measure levels of inflammation or autoantibodies which are usually present in these conditions. In some cases, imaging tests such as X-rays or ultrasounds might be done to assess joint damage caused by psoriasis. Treatment will depend on what type of condition is diagnosed; however common treatments for both eczema and psoriasis include topical medications and phototherapy (light therapy).
6. Is one condition more severe than the other?
No, both conditions are considered to be serious mental health issues. They have different symptoms and treatments, but the severity of each is relative to the individual experience. Depression can range from mild to severe and bipolar disorder can manifest itself as either Type I or Type II. The intensity of these illnesses varies greatly from person to person, making it difficult to compare one against the other in terms of severity. However, since both depression and bipolar disorder can cause significant disruption in a person’s life if left untreated, it is important for individuals who suspect they may have either condition to seek professional help as soon as possible.
7. Are there any triggers that can cause flares in either condition?
For those with IBS, triggers can vary from person to person. Some of the common triggers for a flare-up include eating certain foods, stress, lack of sleep, medications and changes in hormone levels. For those with Crohn’s Disease there are similar triggers including but not limited to smoking, alcohol consumption and certain medications. Other potential causes include bacterial infections or viruses that can cause inflammation in the digestive system leading to flares. In both cases it is important to pay close attention to your body and any potential trigger that could lead to a flare-up so you can take steps to avoid them as much as possible.
8. Does having one condition increase your risk of developing the other?
Having one condition may increase the chance of developing another. This occurs because conditions often share similar risk factors, like genetic predisposition or lifestyle choices. For instance, having type 2 diabetes increases the risk of developing heart disease since they both are linked to an unhealthy diet and lack of physical activity. Additionally, people with autoimmune diseases like rheumatoid arthritis often have higher risks for other autoimmune issues such as lupus or psoriasis due to their shared genetics and immune system imbalances. It’s important that individuals with chronic health issues be mindful of any new symptoms they experience so they can get timely medical attention if necessary.
9 .Are there any long-term complications associated with each disease ?
Yes, each disease comes with its own set of long-term complications. For example, diabetes is associated with a higher risk of developing cardiovascular diseases such as stroke and heart attack due to the damage caused by high blood sugar levels in the body over time. It can also increase your risk for kidney damage, nerve damage and vision loss. Heart disease can cause coronary artery blockage which increases your risk for heart attacks or strokes. Chronic obstructive pulmonary disease (COPD) often causes permanent lung scarring which can lead to irreversible breathing difficulties and reduced quality of life. All these diseases come with their own unique risks that need to be managed over time through regular monitoring, lifestyle changes such as diet and exercise, and potentially medication depending on the severity of the condition.
10 .What is the prognosis for someone who has been diagnosed with either condition ?
The prognosis for someone with either of these conditions will depend on the severity and treatment that is received. For example, if a person has been diagnosed with depression, they may experience some degree of improvement with medication, psychotherapy or lifestyle changes such as exercise or increased social interaction. On the other hand, someone diagnosed with bipolar disorder may require more intensive intervention to manage their symptoms such as mood stabilizers, antipsychotic medications and psychotherapy. In both cases, it is important to find the right course of treatment which can take time but ultimately lead to improved wellbeing and quality of life.